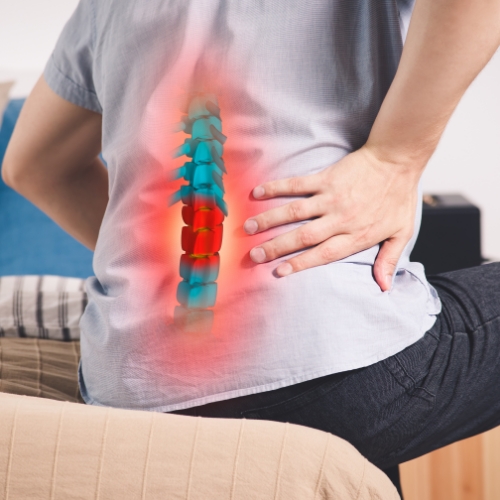
Back pain caused by a slip disc, also known as a herniated or prolapsed disc, occurs when the soft cushion-like material between the spinal bones (vertebrae) bulges or ruptures. This can press on nearby nerves, leading to pain, numbness, or weakness in the back, legs, or even arms, depending on the disc’s location. Common causes include poor posture, heavy lifting, injury, or age-related wear and tear. Physiotherapy plays a vital role in the recovery process. Through manual therapy, strengthening exercises, posture correction, and spinal mobilization, physiotherapy helps reduce pain, restore mobility, and prevent recurrence.Regular sessions and proper guidance can relieve nerve pressure, improve flexibility, and promote a healthy spine for long-term wellness.
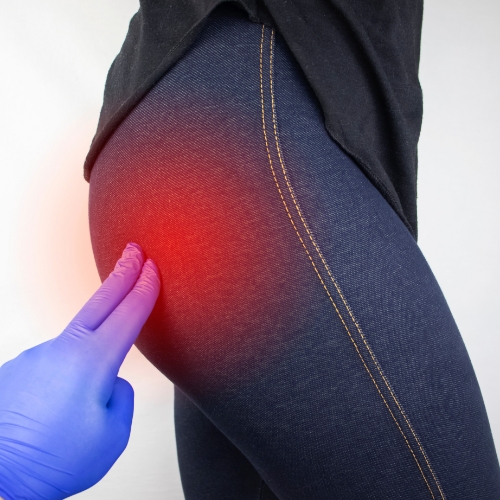
Sciatic pain, or sciatica, occurs when the sciatic nerve — the longest nerve in the body — becomes irritated or compressed. This nerve runs from the lower back through the hips, buttocks, and down each leg. The pain is often sharp, burning, or shooting, and may be accompanied by numbness, tingling, or weakness in the affected leg. Common causes include a slip disc, spinal stenosis, or muscle tightness around the lower back and buttocks. Physiotherapy is highly effective in managing sciatic pain. Treatment focuses on pain relief, nerve mobilization, muscle stretching, and strengthening exercises to reduce pressure on the sciatic nerve. Posture correction and ergonomic advice are also provided to prevent recurrence and help patients regain pain-free movement in daily activities.

Neck pain, often caused by a cervical slip disc, occurs when one of the discs in the cervical spine (neck region) bulges or herniates, pressing on nearby nerves. This can lead to pain, stiffness, tingling, numbness, or weakness in the neck, shoulders, arms, or hands. Poor posture, long hours at a desk, sudden jerks, or age-related degeneration are common contributing factors. Physiotherapy is an effective, non-surgical treatment for cervical disc problems. It includes manual therapy, traction, stretching, strengthening exercises, and posture correction to relieve pressure on the nerves and restore normal neck movement. Regular therapy helps reduce pain, improve flexibility, and prevent future neck strain by promoting better spinal alignment and muscle balance.
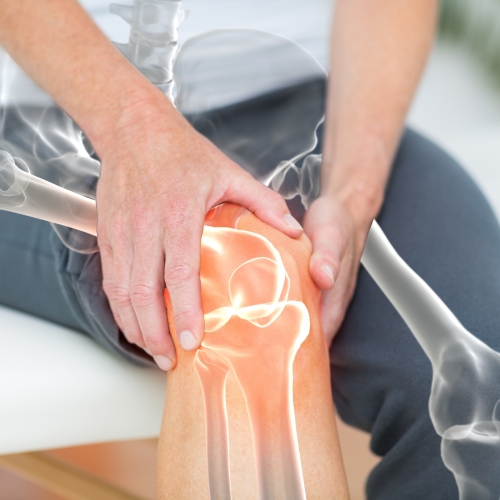
Knee pain due to Osteoarthritis (O.A.) is one of the most common joint problems, especially among older adults. It occurs when the protective cartilage that cushions the ends of the bones in the knee gradually wears away, leading to pain, stiffness, swelling, and reduced movement. Over time, this wear and tear can cause discomfort during walking, climbing stairs, or even simple daily activities. Physiotherapy is a key part of managing knee osteoarthritis. Treatment focuses on strengthening the surrounding muscles, improving joint flexibility, reducing pain, and maintaining mobility. Techniques such as manual therapy, ultrasound, heat therapy, and specific exercises help to ease stiffness and improve function. With regular physiotherapy and lifestyle modifications, patients can maintain joint health and enjoy a more active, pain-free life.

Ankle pain is commonly caused by an ankle sprain, which occurs when the ligaments that support the ankle joint are stretched or torn due to sudden twisting, rolling, or impact. This leads to pain, swelling, bruising, and difficulty in walking or bearing weight. Ankle sprains are frequent in sports or uneven-surface walking and can range from mild ligament strain to severe tears. Physiotherapy plays a crucial role in ankle sprain recovery. Treatment focuses on reducing pain and swelling, followed by restoring strength, flexibility, and balance. Techniques such as ice therapy, ultrasound, gentle mobilization, balance training, and progressive exercises help speed up healing and prevent future injuries. Early physiotherapy ensures proper ligament healing and a safe return to normal or athletic activities.

Hip pain caused by Avascular Necrosis (AVN) occurs when the blood supply to the head of the femur (thigh bone) is reduced or cut off, leading to the death of bone tissue. Over time, this causes the bone to collapse and the hip joint to become painful and stiff. Common causes include injury, long-term steroid use, alcohol abuse, or certain medical conditions. Symptoms often start as mild discomfort in the hip or groin and gradually worsen with movement or weight-bearing. Physiotherapy is essential in managing AVN, especially in the early stages. It helps by reducing pain, maintaining joint mobility, strengthening surrounding muscles, and improving balance and posture. Techniques such as gentle range-of-motion exercises, non-weight-bearing strengthening, hydrotherapy, and gait training are used to preserve joint function. In advanced cases, physiotherapy also aids in post-surgical rehabilitation after procedures like core decompression or total hip replacement to ensure a smooth and strong recovery.
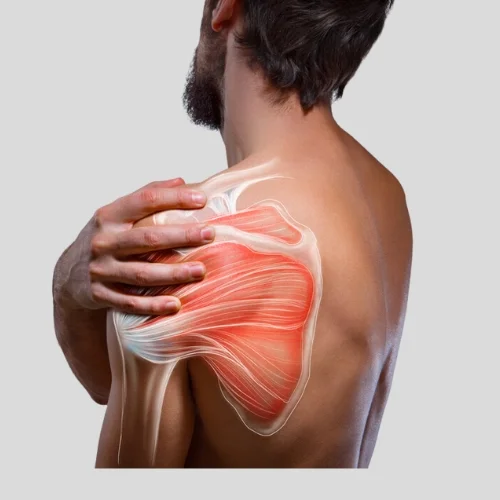
Frozen shoulder, also known as adhesive capsulitis, is a condition that causes stiffness, pain, and limited movement in the shoulder joint. It develops when the connective tissue around the shoulder joint thickens and tightens, restricting motion. The condition often progresses through three stages — freezing (painful phase), frozen (stiff phase), and thawing (recovery phase) — and can last for several months to years. Common causes include prolonged immobilization, diabetes, injury, or post-surgery stiffness. Physiotherapy is the most effective treatment for frozen shoulder. Therapy includes gentle stretching, joint mobilization, heat therapy, and strengthening exercises to restore movement and relieve pain. Regular physiotherapy helps improve shoulder flexibility, reduce stiffness, and restore normal daily function. With consistent care and guided exercises, most patients regain full shoulder mobility over time.
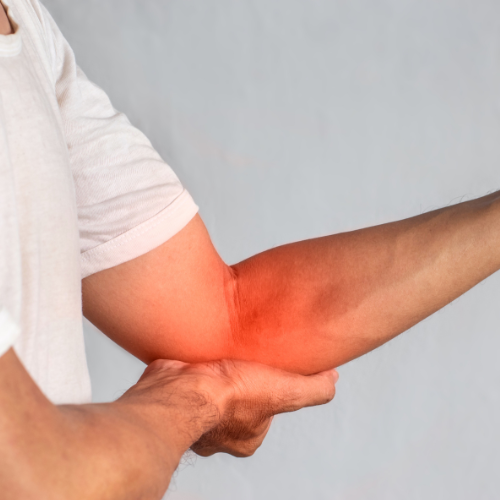
Elbow pain is commonly caused by Tennis Elbow (Lateral Epicondylitis) or Golfer’s Elbow (Medial Epicondylitis) — conditions that result from overuse or repetitive strain on the forearm muscles and tendons attached to the elbow. Tennis elbow affects the outer part of the elbow, while golfer’s elbow affects the inner part. Symptoms include pain, tenderness, weakness in grip, and discomfort during lifting or twisting movements. Physiotherapy is highly effective for both conditions. Treatment involves pain relief techniques, ultrasound therapy, stretching, and strengthening exercises to promote tendon healing. Therapists may also use manual therapy, dry needling, or kinesio taping to reduce strain and support recovery. Proper ergonomic advice and activity modification are provided to prevent recurrence and help restore full, pain-free arm function.
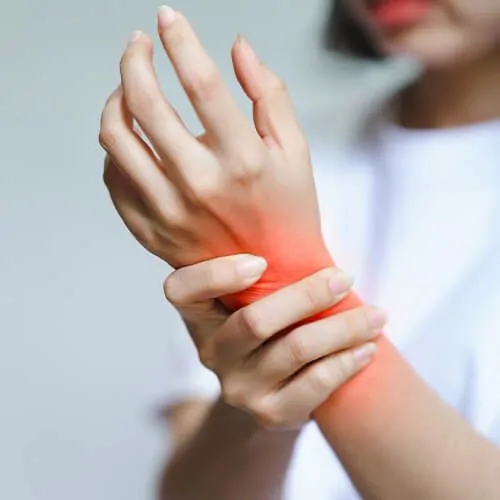
Carpal Tunnel Syndrome (CTS) is a common condition that causes pain, numbness, tingling, and weakness in the wrist and hand. It occurs when the median nerve, which runs through a narrow passage in the wrist called the carpal tunnel, becomes compressed or irritated. Common causes include repetitive wrist movements, prolonged computer use, diabetes, thyroid issues, or wrist injuries. Symptoms often worsen at night or with activities involving gripping or typing. Physiotherapy plays a key role in managing carpal tunnel syndrome. Treatment focuses on reducing nerve compression, relieving pain, and restoring wrist mobility and strength. Techniques such as nerve gliding exercises, stretching, ultrasound therapy, wrist splinting, and posture correction are used to ease symptoms and prevent worsening. With early physiotherapy intervention and ergonomic modifications, most patients experience significant relief and improved hand function.

A stroke occurs when the blood supply to a part of the brain is interrupted or reduced, preventing brain tissue from getting oxygen and nutrients. This leads to the death of brain cells, resulting in paralysis, weakness, loss of coordination, speech difficulties, and other neurological impairments depending on the affected area of the brain. Stroke-related paralysis often affects one side of the body (hemiplegia) and can impact movement, balance, and daily activities. Physiotherapy is a vital part of stroke rehabilitation. It helps patients regain mobility, improve muscle strength, restore balance, and re-learn functional movements. Techniques include neuro-rehabilitation exercises, gait training, balance therapy, and task-specific training. Consistent therapy not only promotes physical recovery but also helps improve confidence and independence in daily life. Early and continuous physiotherapy greatly enhances the chances of long-term recovery and quality of life after a stroke

Facial palsy, commonly known as Bell’s palsy, is a condition that causes sudden weakness or paralysis of the muscles on one side of the face. It occurs due to inflammation or compression of the facial nerve (7th cranial nerve), which controls facial movements. The exact cause is often unknown but may be linked to viral infections, stress, or exposure to cold air. Symptoms include drooping of one side of the face, difficulty closing the eye, drooling, loss of facial expression, and sometimes altered taste or tear production. Physiotherapy plays a crucial role in recovery from Bell’s palsy. Treatment focuses on facial muscle re-education, gentle exercises, massage, electrical stimulation, and mirror therapy to improve muscle tone and coordination. Early therapy helps prevent muscle stiffness and facial asymmetry, promoting faster and more complete recovery. With consistent physiotherapy and care, most patients regain normal facial movement and expression over time.

Parkinson’s disease is a progressive neurological disorder that affects movement and coordination. It occurs due to a loss of dopamine-producing cells in a part of the brain called the substantia nigra. Common symptoms include tremors (shaking), muscle stiffness, slowness of movement (bradykinesia), balance problems, and changes in speech or handwriting. As the condition progresses, it can also affect facial expression and walking pattern. Physiotherapy is an important part of managing Parkinson’s disease. It helps patients maintain mobility, improve balance, strengthen muscles, and enhance posture and flexibility. Techniques such as gait training, balance exercises, rhythmic movement therapy, and relaxation techniques are used to improve daily functioning and confidence. Regular physiotherapy sessions, along with medication and lifestyle changes, help individuals with Parkinson’s lead more active, independent, and fulfilling lives.
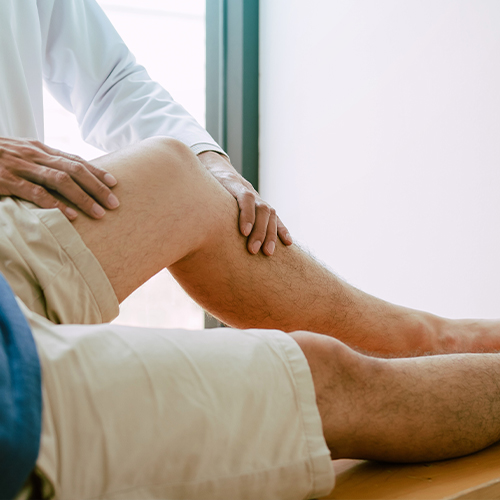
A ligament injury occurs when the tough, fibrous bands of tissue that connect bones to each other are stretched, partially torn, or completely ruptured. This often happens due to sudden twisting, impact, or overstretching, commonly seen in sports, falls, or accidents. Symptoms include pain, swelling, bruising, instability, and difficulty in moving the affected joint. Common sites of ligament injuries include the knee (ACL, MCL), ankle, wrist, and shoulder. Physiotherapy plays a vital role in the recovery and rehabilitation of ligament injuries. Treatment focuses on reducing pain and swelling, restoring joint mobility, strengthening surrounding muscles, and improving stability and balance. Techniques such as ice therapy, ultrasound, manual therapy, and progressive strengthening exercises are used. In severe cases (after surgical repair), physiotherapy ensures safe and effective post-operative rehabilitation, helping patients return to normal activities and sports with confidence.

Guillain-Barré Syndrome (GBS) is a rare neurological disorder in which the body’s immune system attacks the peripheral nerves, leading to muscle weakness, numbness, and sometimes paralysis. The condition often starts with tingling or weakness in the legs and can progress to affect the arms, face, and even breathing muscles. GBS can develop after viral or bacterial infections, vaccinations, or surgery. Although the exact cause is unknown, it is considered an autoimmune response. Physiotherapy is an essential part of GBS rehabilitation. In the early stages, therapy focuses on preventing joint stiffness, maintaining circulation, and avoiding muscle contractures through gentle passive movements. As recovery progresses, active exercises, strengthening, balance training, and gait re-education are introduced to rebuild muscle strength and coordination. Regular physiotherapy helps patients restore mobility, improve independence, and enhance overall quality of life during and after recovery.
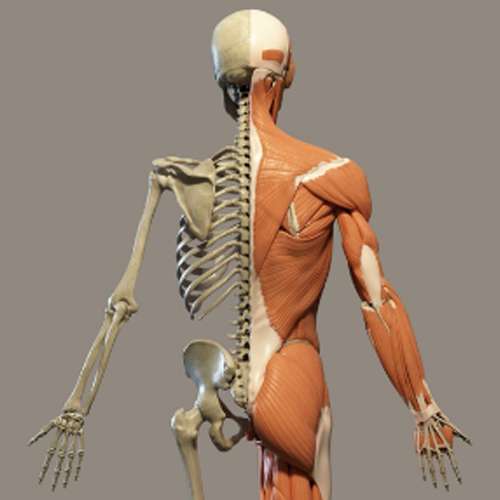
Muscular atrophy refers to the loss or wasting away of muscle tissue, leading to weakness, reduced strength, and limited movement. It can result from prolonged inactivity, nerve injury, aging, malnutrition, or certain medical conditions such as stroke, spinal cord injury, or neuromuscular disorders. When muscles are not used regularly, they gradually shrink and lose their ability to function effectively. Physiotherapy is crucial in managing muscular atrophy. The goal is to rebuild muscle strength, improve flexibility, and restore functional movement. Treatment includes resistance training, electrical muscle stimulation, stretching, postural correction, and progressive exercise programs tailored to the patient’s condition. With consistent physiotherapy and proper nutrition, muscle tone and strength can be improved, helping patients regain mobility, independence, and better quality of life.
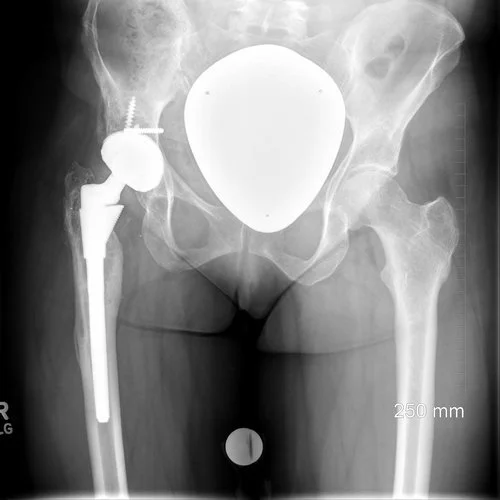
Total Hip Replacement (THR) is a surgical procedure in which a damaged or diseased hip joint is replaced with an artificial implant made of metal, ceramic, or plastic components. It is commonly performed in cases of severe arthritis, avascular necrosis (AVN), fractures, or chronic hip pain that limit movement and daily activities. After surgery, patients may experience stiffness, pain, or difficulty walking, which requires proper rehabilitation. Physiotherapy plays a vital role in recovery after THR. Post-surgical therapy focuses on reducing pain and swelling, restoring joint movement, strengthening the hip and leg muscles, and improving balance and walking patterns. Techniques include gentle range-of-motion exercises, gait training with assistive devices, and progressive strengthening programs. Regular physiotherapy helps patients regain mobility, independence, and confidence, ensuring a safe return to daily and active life.
Total Knee Replacement (TKR) is a surgical procedure in which a damaged or worn-out knee joint is replaced with an artificial implant made of metal and plastic components. It is usually recommended for patients suffering from severe osteoarthritis, rheumatoid arthritis, or post-traumatic knee damage that causes chronic pain, stiffness, and difficulty in walking or performing daily activities. Physiotherapy after TKR is essential for a successful recovery. It focuses on pain management, restoring knee movement, strengthening leg muscles, and improving balance and walking ability. Early rehabilitation includes gentle range-of-motion exercises, quadriceps strengthening, gait training, and functional activities. Consistent physiotherapy helps reduce swelling, enhance flexibility, and ensure proper joint alignment, allowing patients to return to normal activities with improved comfort, stability, and confidence.
Sports injuries are common among athletes and active individuals and occur due to sudden impact, overuse, or improper technique during physical activity. These injuries can affect muscles, ligaments, tendons, joints, or bones, leading to pain, swelling, bruising, reduced mobility, and sometimes long-term functional limitations. Common examples include sprains, strains, fractures, dislocations, and tendon injuries. Physiotherapy plays a critical role in the treatment and rehabilitation of sports injuries. Therapy focuses on reducing pain and inflammation, restoring strength, flexibility, and range of motion, and preventing recurrence. Techniques include manual therapy, therapeutic exercises, taping, electrotherapy, and sport-specific training. With proper physiotherapy, athletes can recover safely, regain optimal performance, and return to their sport confidently, minimizing the risk of future injuries.

Electro Therapy is an advanced physiotherapy technique that uses mild electrical currents to reduce pain, improve muscle strength, and speed up recovery. It helps stimulate nerves and muscles, enhances blood circulation, and decreases inflammation in the affected area. Commonly used for back pain, arthritis, muscle spasms, and sports injuries, this therapy provides a safe and effective way to restore normal movement and function without medication. Electro Therapy is a painless and non-invasive treatment that helps relieve pain and promote faster healing. By sending gentle electrical impulses to the affected muscles and nerves, it reduces swelling, improves blood flow, and supports natural recovery. It is especially helpful for joint pain, muscle weakness, and nerve problems.
TENS therapy is a safe and effective pain-relief technique that uses low-voltage electrical currents to stimulate the nerves and reduce pain signals to the brain. It helps relieve chronic pain, muscle tension, and nerve-related discomfort. Commonly used for back pain, arthritis, and post-surgical recovery, TENS therapy promotes relaxation and enhances the body’s natural healing process. IFT therapy is an advanced electrotherapy treatment designed to reduce pain, swelling, and inflammation deep within the tissues. It works by sending medium-frequency electrical currents that penetrate muscles and joints more effectively than traditional methods. Ideal for muscle spasms, joint stiffness, and sports injuries, IFT improves blood flow, reduces pain, and accelerates recovery.

Wax Therapy, also known as Paraffin Wax Treatment, is a popular physiotherapy technique used to relieve joint and muscle pain, improve blood circulation, and relax stiff muscles. During the treatment, warm paraffin wax is applied to the affected area, providing deep heat that softens tissues, reduces stiffness, and increases mobility. It is especially beneficial for conditions like arthritis, joint pain, muscle tightness, and post-injury stiffness. Safe, soothing, and highly effective, wax therapy offers both pain relief and relaxation, making it a preferred choice for many patients. Wax Therapy uses warm paraffin wax to gently heat the affected area, providing instant comfort and relief from pain and stiffness. It helps loosen tight joints, relax sore muscles, and improve skin texture. Commonly used for hands, feet, and elbows, this soothing therapy leaves you feeling relaxed and refreshed.
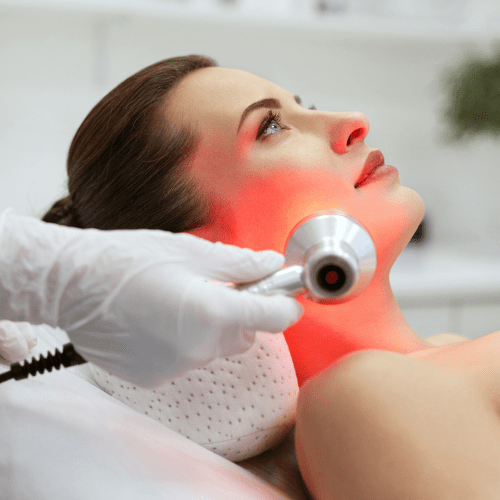
nfrared (IR) Therapy is a heat-based physiotherapy treatment that uses infrared light to penetrate deep into the muscles, tissues, and joints. This gentle heat improves blood circulation, reduces stiffness, and relieves muscle and joint pain. It is highly effective for conditions like arthritis, back pain, muscle spasms, and sports injuries. IR therapy promotes relaxation, enhances healing, and helps restore natural movement without any side effects. IR Therapy uses soothing infrared light to warm the affected area, helping reduce pain, stiffness, and muscle tension. The deep heat improves blood flow and supports faster healing of tissues. It’s a safe and comfortable treatment often used for back pain, arthritis, and muscle soreness.
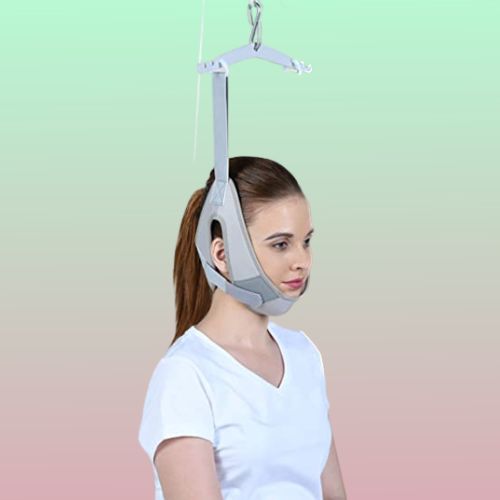
Cervical Traction Therapy is an effective treatment used to relieve neck pain, stiffness, and nerve compression by gently stretching the cervical spine. This helps reduce pressure on spinal discs, improve posture, and relax neck muscles. It is highly beneficial for patients suffering from cervical spondylosis, slipped disc, and nerve root compression. The therapy enhances blood flow, reduces muscle tension, and restores normal neck mobility safely and effectively. Cervical Traction gently stretches the neck to relieve pressure on the spine and nerves. It helps reduce neck pain, muscle tightness, and stiffness, allowing better movement and comfort. This therapy is ideal for people with cervical spondylosis, slip disc, or constant neck strain from posture issues.

Lumbar Traction Therapy is a specialized physiotherapy treatment used to relieve lower back pain by gently stretching the lumbar spine. This process helps reduce pressure on spinal discs and nerves, promoting proper alignment and relaxation of tight muscles. It is especially beneficial for conditions such as slip disc, sciatica, lumbar spondylosis, and chronic lower back pain. The therapy improves blood circulation, reduces stiffness, and supports long-term spinal health. Lumbar Traction helps relieve lower back pain by gently pulling and stretching the spine. This reduces pressure on nerves and discs, relaxes muscles, and improves movement. It’s a safe and effective treatment for slip disc, sciatica, and back stiffness, helping patients recover naturally without surgery.